Learning at the point of care: specialist nursing burns placement at a major Trauma Centre
20 Feb 2026
Written by Erika Lu
Strengthening specialist capability is central to the National Critical Care and Trauma Response Centre’s (NCCTRC) approach to preparedness. Placement opportunities upskill and equip clinicians to operate confidently in complex high-acuity environments.
For Acting Trauma Coordinator Karen Kampana, this meant undertaking a specialist burns placement at The Alfred Hospital Victorian Adult Burns Service (VABS), a level I Major Trauma Centre and a statewide provider of adult burns care.

NCCTRC Acting Trauma Coordinator Karen Kampana (right) with Mel Neely, Burns Nurse Clinical Lead at The Alfred Hospital’s Victorian Adult Burns Service.
Karen has been a registered nurse at the Royal Darwin Hospital (RDH) for 14 years. Supported by the NCCTRC, the RDH is a level II Trauma Centre and the only one in the Northern Territory (NT). The Trauma Service team delivers care for remote and complex trauma across a vast geographical area of approximately 1.35 million squared kilometres, covering some of the most remote communities in Australia, where patients often present with rapidly evolving risks that require coordinated, high-acuity trauma care.
The placement provided Karen with deeper insight into the leadership structures, staffing models and multidisciplinary workflows of a major burns centre.
“Working within the specialist burns centre highlighted how critical preparation and multidisciplinary coordination are in high-acuity care,” Karen said.
The 3-week placement enhanced my clinical skills and confidence in managing complex and unpredictable situations.
Karen participated in major burns resuscitations in the Emergency Department focusing on patient assessment, management and care. She also observed burns theatre procedures, including wound debridement and skin grafting, and cared for patients with large total body surface area (TBSA) burns in the intensive care unit (ICU).
“With the guidance and support of the Burns Liaison Nurses, I developed skills in planning, assessing and assisting with complex wound management, including Biobrane, Biodegradable Temporizing Matrix (BTM), Meek graft and human skin equivalent dressings.”
Participation in daily ward rounds, scheduled dressings under sedation (DUS), outpatient burns clinics and multidisciplinary simulations further expanded her understanding of coordinated, patient-centred care across the continuum.
“Seeing the patient journey from resuscitation through to rehabilitation emphasised the importance of continuity of care in burns management,” she reflects. “The level of coordination between teams was exceptional – clear communication and shared clinical understanding are essential when managing complex trauma.”
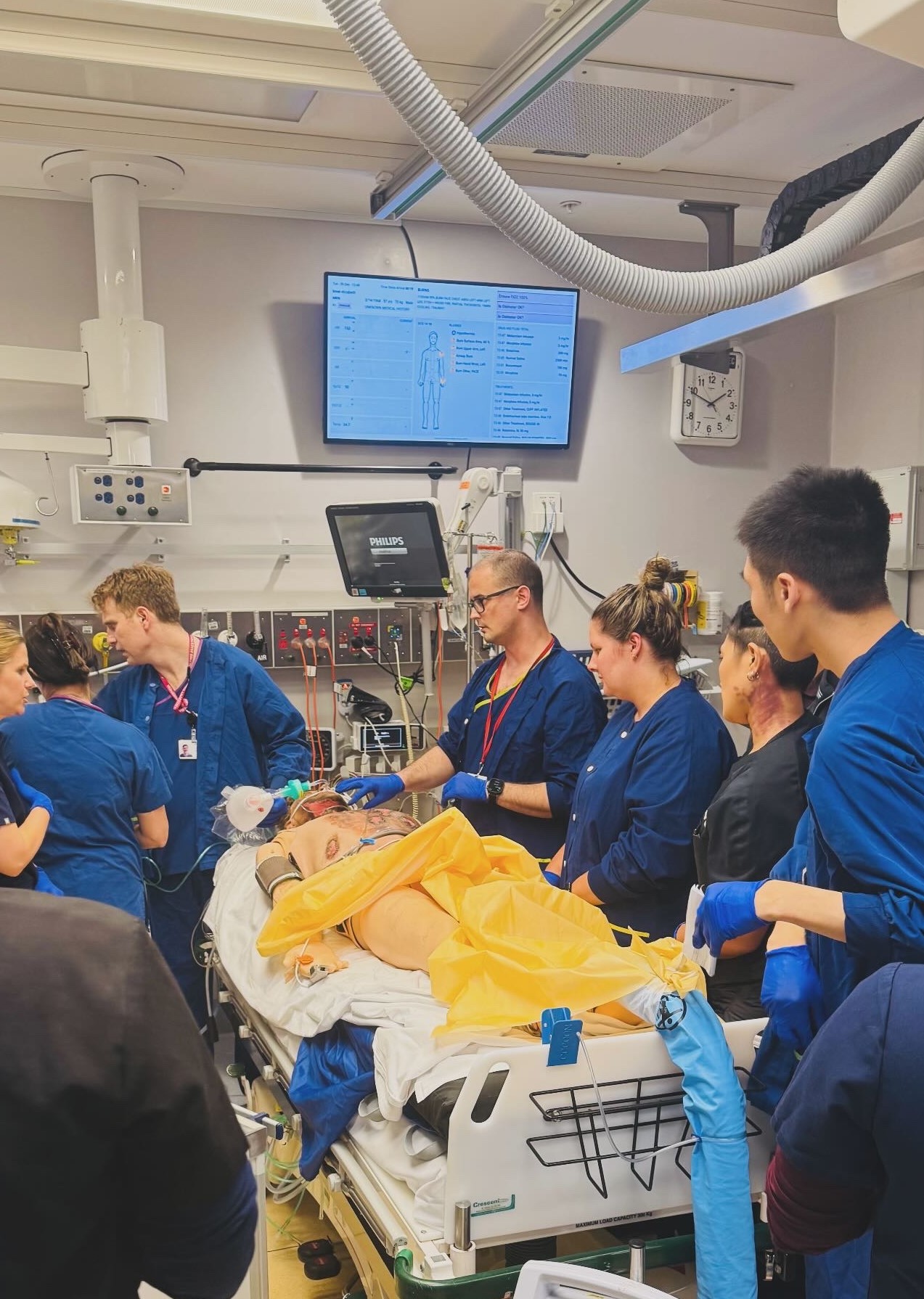
A major burns multidisciplinary team simulation at The Alfred Hospital.
Key learning outcomes
1. Advanced clinical capability
Developed advanced skills in patient assessment, decision-making and clinical procedures across emergency, critical care and ward environments.
2. Multidisciplinary coordination and operational insight
Gained first-hand experience working within an integrated care model involving medical, nursing and allied health teams, supported by defined leadership and staffing structures in a level I Major Trauma Service.
3. Critical decision-making and continuity of care in high-acuity environments
Refined the ability to prioritise care and make timely clinical decisions in complex, high-pressure scenarios.
Impact and outcome
Karen’s placement directly supports the development of the Burns Service at the RDH.
“Like Karen, nurses from specialty areas such as the ICU and Operating Theatre are also upskilling to better manage major burns locally, particularly during the critical period before transfer to a specialist centre when needed,” Acting Trauma Nursing Director Belinda Nolan shared.
Exposure to the systems and models of care used in a major burns centre supports shared clinical structures aligned with the Australian and New Zealand Burns Association (ANZBA) and the Emergency Management of Severe Burns (EMSB) standards, improving the interoperability across the Surgery and Critical Care Division, Trauma Service and Burns Service.
“At a broader level, advancing burns capability adds depth to AUSMAT’s deployable workforce and supports readiness for high-acuity, trauma-heavy health emergency responses,” Belinda added. “Enhanced specialist capability in the NT contributes to national surge capacity and collective readiness.”
The placement also strengthens collaboration among the NCCTRC, RDH and The Alfred Hospital through shared clinical language, aligned standards and professional relationships that are crucial during multi-centre responses.



Karen Kampana with The Alfred Hospital Burns Team and the Royal Children's Hospital Trauma Service during her specialist burns placement.
For Karen, the placement was both professionally and clinically challenging.
“It was an incredible learning experience that boosted my confidence and highlighted the importance of preparation, teamwork and specialist capability,” she added.
Funded by the Australian Government, the NCCTRC supports the coordinated systems and workforce capability that strengthen healthcare delivery for complex trauma and major burns.












