Understanding and managing avian influenza risk
06 Mar 2026
Written by Dr Bhavya Balasubramanya and Dr Sophia Bowman-Derrick
The virus
Avian influenza or ‘bird flu’ is caused by strains of the Influenza A virus that typically infect birds. It is classified according to 2 surface molecules – haemagglutinin (HA) and neuraminidase (NA). Scientists have identified 17 HA subtypes and 9 NA subtypes.
These viruses are further classified by their impact on poultry. Low pathogenicity avian influenza (LPAI) is common in wild birds and usually causes little or no illness, while high pathogenicity avian influenza (HPAI) can cause severe disease and mortality rates of up to 100% in affected flocks.
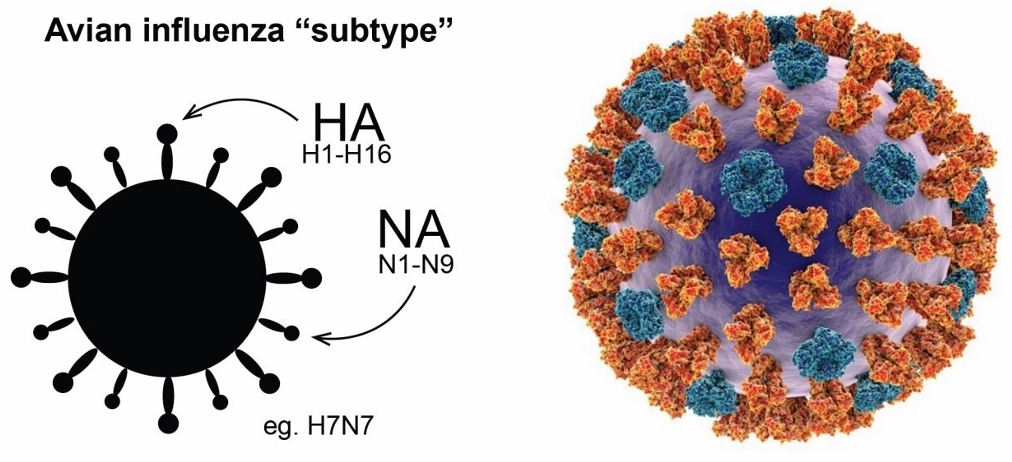
Figure 1. Avian influenza subtype. Michelle Wille via Wildlife Health Australia.
These viruses can evolve rapidly. Notably, H5 and H7 subtypes can mutate from LPAI to HPAI. The current dominant global strain of avian influenza is H5, which includes several variants with different NA subtypes.
Managing its spread requires a One Health approach, recognising the interconnected health of humans, animals and the environment.
Public health significance
While avian influenza rarely infects humans, people with close contact with birds face an increased risk of infection. Outbreaks in poultry can cause mass mortality and often require the culling of healthy birds to contain further spread.
Beyond animal health, avian influenza can have significant economic and social impacts. In developing countries where poultry farming is labour-intensive, outbreaks and flock losses can result in substantial job losses. HPAI also disrupts international trade in live birds and poultry products, affecting national economies and food security.
Dr Elly Layton, NCCTRC’s Public Health Medical Officer, contributed to the May 2024 Victorian H7 avian influenza response during her time with the state's Department of Health. The outbreak resulted in the destruction of approximately 1.3 million birds and contributed to national egg shortages.
“Supporting the bird flu response activities showed me how quickly these situations can evolve,” Dr Layton shared.
Within a month, there were 8 farms infected and hundreds of poultry workers potentially exposed.
"Working collaboratively with agriculture colleagues to rapidly undertake a risk assessment and implement coordinated public health control measures were essential in protecting the broader community," Dr Layton added.
Epidemiology
Wildlife
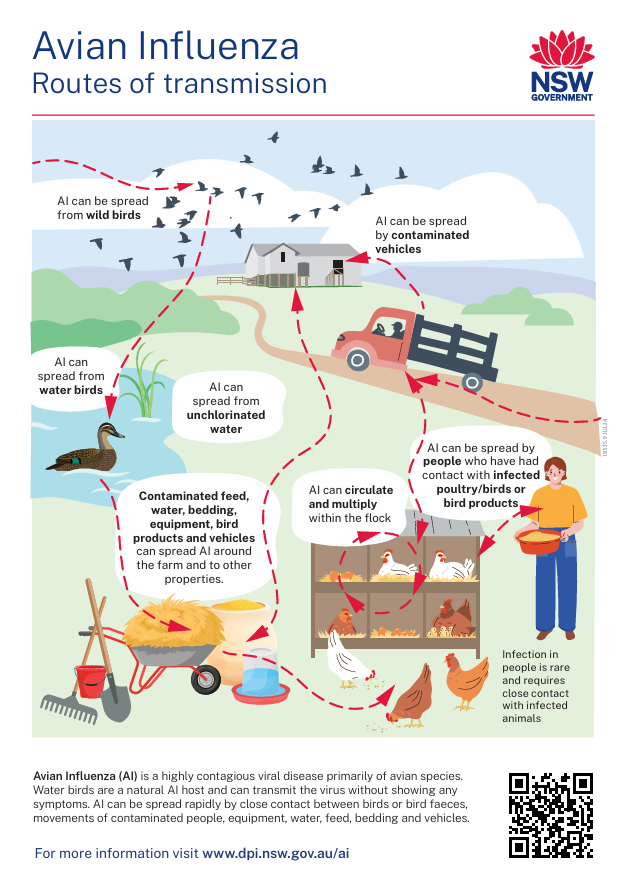
Wild waterbirds – such as ducks, swans, geese, terns, gulls and shorebirds – are the primary natural reservoirs of avian influenza. These birds often carry LPAI without showing signs of illness and can shed the virus through faeces and respiratory secretions, contributing to its global spread. LPAI can transmit from wild birds to domestic poultry, where strains may mutate into HPAI and cause severe disease and high mortality.
Figure 2. Avian influenza routes of transmission. New South Wales Government.
Domestic animals
Poultry infected by H5 avian influenza can show a drop in egg production, lethargy, swelling of the head or legs, bruising, breathing issues or sudden death.
Infected mammals may show signs of tiredness, difficulty walking, seizures, tremors, drooling, runny nose or sudden death. Mammals known to have been infected include pigs, horses, cattle, dogs and cats, although these infections remain relatively uncommon.
Humans
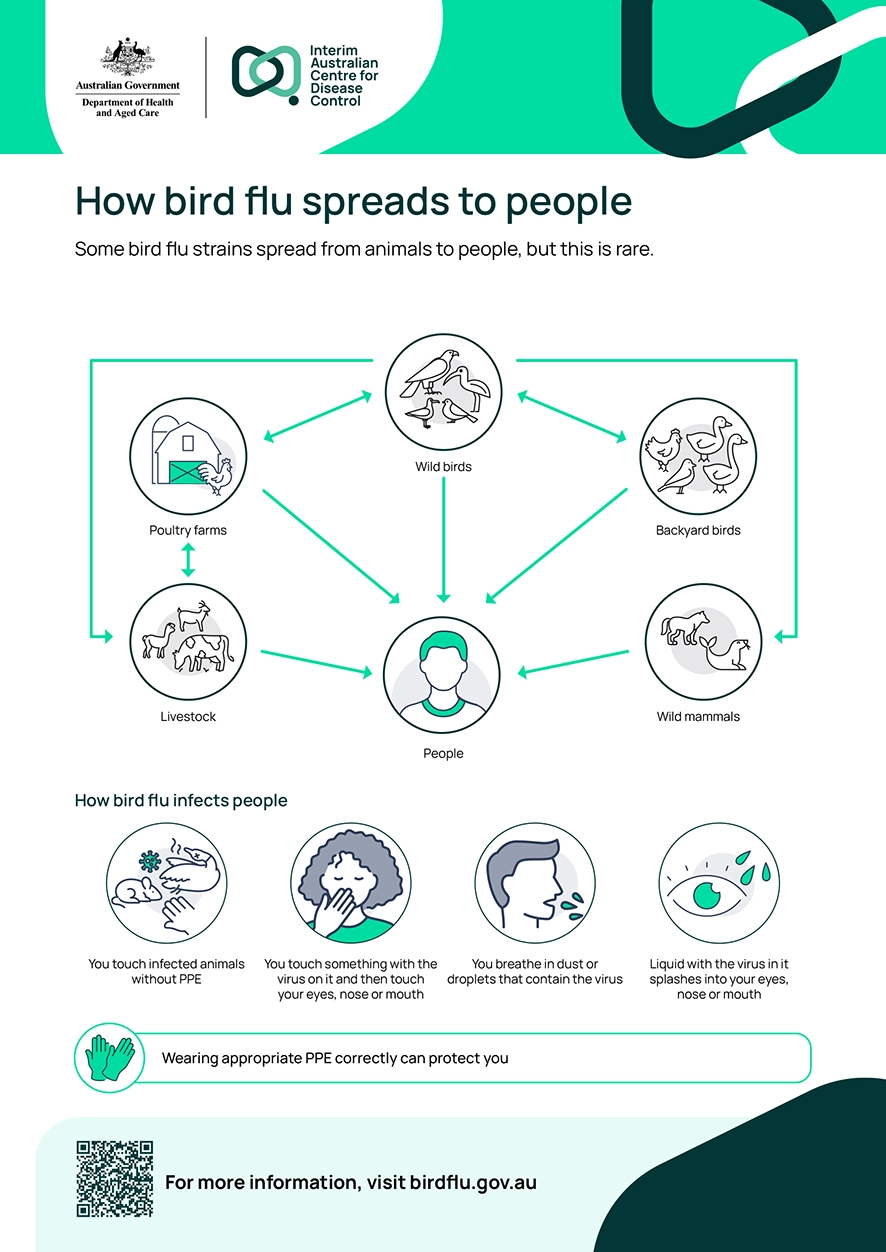
The first recognised human infections with the H5N1 strain of avian influenza occurred in 1997 during an outbreak in poultry in Hong Kong. Humans are most often infected after close contact with infected poultry. Other risk factors include handling carcasses of infected poultry and preparing infected poultry for consumption.
Figure 3. How bird flu spreads to people. Australian Government Department of Health and Aged Care.
Infection in humans may be asymptomatic or cause flu-like symptoms including fever, cough, tiredness, muscle aches, sore throat, shortness of breath, runny nose, headache or diarrhoea. Severe cases may progress to pneumonia, encephalitis and death.
“Symptoms of avian influenza can be similar to the seasonal flu, so a specific test for avian influenza may not always be conducted,” Dr Layton said. “Determining if someone has had contact with infected poultry is an essential part of making the diagnosis.”
The incubation period for avian influenza infection in humans varies by strain, typically ranging from 1-10 days. People may remain infectious until approximately 7 days after symptoms appear, although sustained human-to-human transmission has not been observed. Diagnosis is confirmed through laboratory testing of a nose or throat swab, or sputum sample.
Global distribution
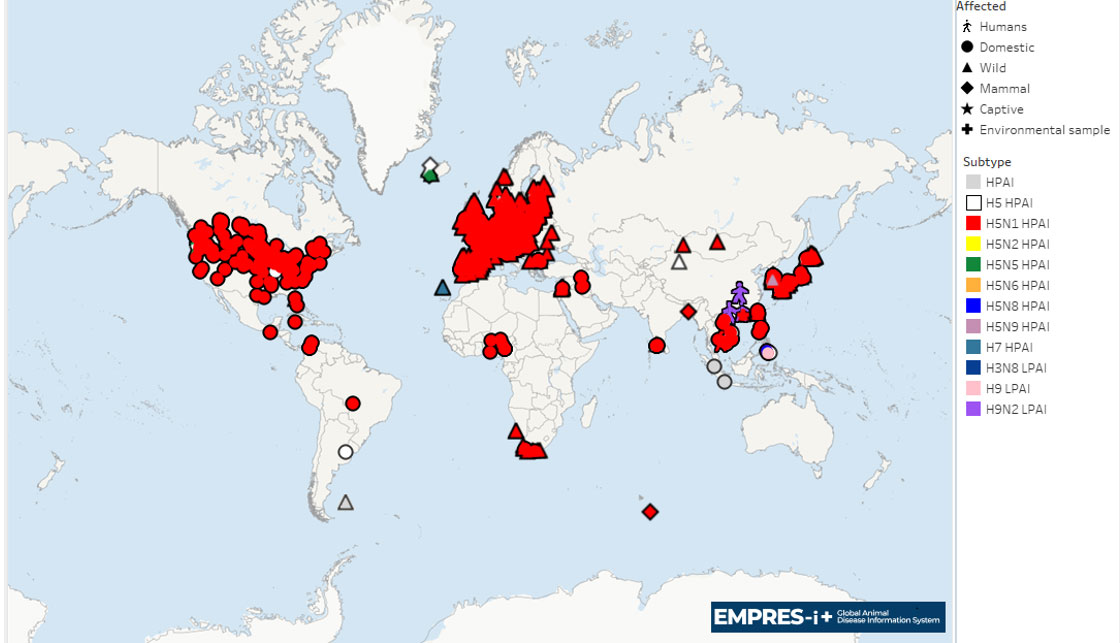
The H5 strain has spread globally through migratory bird movements. Between 2021 and 2023, there were 8,203 outbreaks of high pathogenicity avian influenza (HPAI) in poultry across all regions except Australia and New Zealand. Since 1 January 2003, 993 human cases have been reported in 25 countries, resulting in 447 fatalities.
Figure 4: Global distribution of avian influenza with zoonotic potential observed since 1 October 2005. Food and Agriculture Organization of the United Nations.
Public health response
One Health is an integrated approach which recognises the interconnected health of humans, animals and the environment and is essential in managing the ongoing risk of HPAI.
The global public health response is guided by the following organisations.
- World Organisation for Animal Health (WOAH) collects and disseminates official animal disease information from member countries, collaborates with national veterinary services and provides technical assistance. WOAH member countries report detection of HPAI to the WOAH Information System, the global animal health reference database.
- World Health Organization (WHO) monitors avian and other zoonotic influenza viruses through its Global Influenza Surveillance and Response System (GISRS). WHO has published the Influenza (Avian and other zoonotic) Outbreak Toolbox which includes protocols for investigation, case definitions, data collection tools and specimen collection procedures.
- Food and Agriculture Organisation (FAO) publishes resources to help countries respond to avian influenza outbreaks.
- Joint WOAH-FAO Scientific Network on Animal Influenza (OFFLU) is a global network of experts that fosters collaboration between animal and human health specialists.
The public health response to avian influenza requires collaboration with human and animal health colleagues to undertake prevention, surveillance and outbreak management.
Key components
Animals
- Strict biosecurity and good hygiene practices
- Measures to prevent contact between poultry and wild birds
- Quarantining new birds before introducing them to existing birds
- Bird owners and farmers need to monitor their birds for signs of avian influenza
Environment
- Treat drinking water supplied from open surface water to minimise potential risks to human and animals
- Ensure dead animals are appropriately buried
People
- Annual seasonal influenza vaccination to reduce the chance of simultaneous infection with human and avian influenza, which could allow the viruses to mutate
- Avoid poultry farms and live bird markets in regions with avian influenza
- Wash hands after touching uncooked poultry products
- Ensure poultry and poultry products are well-cooked prior to consumption
- If working with poultry, wear personal protective equipment
- If working with poultry and you develop signs of avian influenza, isolate from others and seek urgent medical advice
Animals
- Any detection of avian influenza in birds must be notified to the local state or territory animal health authorities
- Monitoring of avian influenza in wild birds, for example, Wildlife Health Australia operates a national program, the National Avian Influenza Wild Bird (NAIWB) Steering Group which coordinates national surveillance
People
- Monitor the health of people exposed to animals with influenza
- Investigate all suspected cases of zoonotic influenza
- All cases of zoonotic influenza should be reported to WHO under the International Health Regulations
Animals
- Infected animals and those in close contact are culled to rapidly contain and eradicate avian influenza
- Vaccination of poultry may be recommended under specific conditions as part of a disease control strategy, for example during outbreaks in a country previously free of the virus
People
- In human infections, assess exposure to animals and travel history, undertake contact tracing and early identification of any unusual respiratory events
- Those involved in poultry culling and cleaning must wear appropriate personal protective equipment
- All staff involved in culling infected poultry should have their health status monitored for 7 days following exposure
- Staff likely to have been exposed to avian influenza should receive the seasonal influenza vaccine
References
- Animal Health Australia. Avian influenza. https://animalhealthaustralia.com.au/resources/threat-updates/avian-influenza/
- Australian Government Department of Agriculture, Fisheries and Forestry. Avian influenza. https://www.agriculture.gov.au/biosecurity-trade/pests-diseases-weeds/animal/avian-influenza/about
- Australian Government Department of Agriculture, Fisheries and Forestry. Bird owners and bird flu. https://www.agriculture.gov.au/biosecurity-trade/pests-diseases-weeds/animal/avian-influenza/help-protect/bird-owners
- Australian Government Department of Agriculture, Fisheries and Forestry. What we are doing to prepare for bird flu. https://www.agriculture.gov.au/biosecurity-trade/pests-diseases-weeds/animal/avian-influenza/government-action
- Australian Centre for Disease Control (2024) Communicable Diseases Network Australia National guidelines for avian influenza: protecting people who work with birds and wildlife, published by. National guidelines for avian influenza – protecting people who work with birds and wildlife
- Food and Agriculture Organisation (2006) Preparing for highly pathogenic avian influenza. https://openknowledge.fao.org/server/api/core/bitstreams/6f79f597-d7a0-4f57-be15-376f0d427371/content
- Food and Agriculture Organisation (2026) Global Avian Influenza Viruses with Zoonotic Potential situation update. https://www.fao.org/animal-health/situation-updates/global-aiv-with-zoonotic-potential/en
- Government of South Australia SA Health (2025) Avian Influenza (bird flu) in humans - including symptoms, treatment and prevention. https://www.sahealth.sa.gov.au/wps/wcm/connect/public+content/sa+health+internet/conditions/infectious+diseases/flu/avian+flu
- Wildlife Health Australia (2025) Avian influenza in wild birds in Australia – Fact Sheet, published by Wildlife Health Australia. pdf
- Wildlife Health Australia Resource Centre. H5 bird flu. https://wildlifehealthaustralia.com.au/Resource-Centre/H5-bird-flu
- Wildlife Health Australia (2025) Technical Update: Global High Pathogenicity Avian Influenza in Wildlife. https://wildlifehealthaustralia.com.au/Portals/0/Incidents/HPAI_Technical_Update.pdf
- Wildlife Health Australia. Wild Bird Surveillance. https://wildlifehealthaustralia.com.au/Our-Work/Surveillance/Wild-Bird-Surveillance
- World Health Organization (2026) Influenza (avian and other zoonotic). https://www.who.int/news-room/fact-sheets/detail/influenza-(avian-and-other-zoonotic)
- World Organisation for Animal Health. Avian influenza. https://www.woah.org/en/disease/avian-influenza/
- World Organisation for Animal Health WAHIS: World Animal Health Information System. https://wahis.woah.org/#/home
- World Health Organization Avian Influenza Weekly Update Number 1029 (2026). https://cdn.who.int/media/docs/default-source/wpro---documents/emergency/surveillance/avian-influenza/ai_20260116.pdf